Hysteroscopy in Chennai
Diagnostic and operative hysteroscopy in Chennai by Dr. Rukkayal — direct visualisation of the uterine cavity to identify and treat polyps, fibroids, adhesions, and septae that affect fertility and pregnancy outcomes.

Hysteroscopy is a minimally invasive procedure that allows direct visual examination of the uterine cavity through the cervix — with no abdominal incisions. For women preparing for IVF, struggling with implantation failure, experiencing abnormal bleeding, or coping with recurrent miscarriage, hysteroscopy frequently uncovers and corrects intracavitary problems that standard ultrasound and even HSG can miss. Dr. Rukkayal performs both diagnostic and operative hysteroscopy as part of a fertility-focused workup, ensuring uterine findings translate directly into a tailored next step.
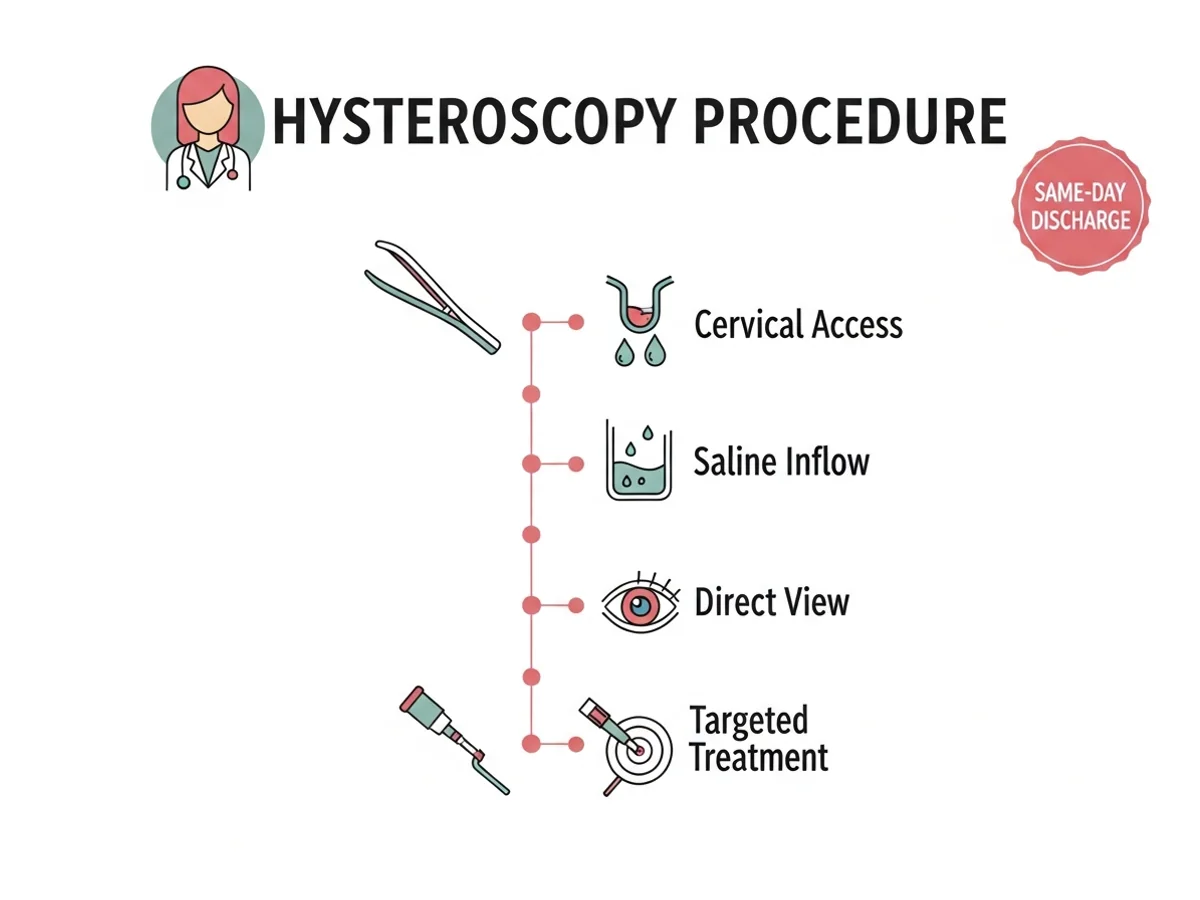
A slender camera (hysteroscope) is gently passed through the cervix while saline distends the uterine cavity, giving a magnified, high-definition view of the endometrium and the openings of the fallopian tubes. Polyps, submucosal fibroids, intrauterine adhesions (Asherman syndrome), and uterine septae can be identified and, in most cases, treated in the same sitting. Because there are no abdominal incisions, most patients are discharged the same day, have minimal pain, and return to normal activity within 24 to 48 hours. For women undergoing IVF, addressing even subtle uterine cavity abnormalities before embryo transfer can meaningfully improve implantation and live-birth rates. Dr. Rukkayal’s combined MRCOG (UK) and FRM (Germany) training brings a fertility-first lens to every hysteroscopy — every finding is interpreted in the context of what it means for your next embryo transfer or natural conception attempt.
800+
Hysteroscopies Performed
>95%
Same-Day Discharge
When Is Hysteroscopy Recommended?
You should see a specialist if you experience:
- Recurrent IVF or embryo transfer failure
- Abnormal findings on ultrasound suggesting a polyp or fibroid
- Heavy, prolonged, or irregular periods
- Recurrent miscarriage with suspected uterine factor
- Suspected intrauterine adhesions after previous surgery or infection
- Suspected uterine septum on 3D ultrasound or MRI
- Bleeding after menopause
Understanding Hysteroscopy
Hysteroscopy is considered the reference standard for evaluating the uterine cavity because it allows direct visualisation rather than indirect imaging. Diagnostic hysteroscopy is brief (10–15 minutes) and can often be performed under sedation; operative hysteroscopy uses specialised instruments passed through the same scope to remove polyps, resect submucosal fibroids, divide adhesions, or correct a uterine septum. Compared with traditional dilatation and curettage (D&C), hysteroscopy is targeted rather than blind — meaning tissue is removed only where it should be, sparing the healthy endometrium that future embryos will implant into. The procedure is performed using saline or glycine as the distension medium, with no radiation and no risk to ovarian reserve.
Uterine Conditions We Treat

Hysteroscopic Procedures We Perform
Diagnostic Hysteroscopy
A short outpatient procedure to evaluate the uterine cavity and tubal openings. Often performed before IVF, after recurrent miscarriage, or to confirm findings seen on ultrasound. Frequently combined with an endometrial biopsy.
Hysteroscopic Polypectomy
Precise removal of endometrial polyps under direct vision. Polyps are a common but often overlooked cause of subfertility, abnormal bleeding, and recurrent miscarriage — removing them can restore a healthy implantation environment.
Hysteroscopic Myomectomy
Resection of submucosal fibroids (those growing into the uterine cavity) using specialised resectoscopes. Removing these fibroids before IVF or pregnancy is consistently associated with improved fertility and reduced miscarriage risk.
Adhesiolysis for Asherman Syndrome
Careful division of intrauterine adhesions caused by previous D&C, infection, or surgery. Post-procedure oestrogen therapy and short-term uterine stenting may be used to keep the cavity open while the lining regenerates.
Septum Resection
Correction of a uterine septum — a congenital partition that increases miscarriage risk — using hysteroscopic scissors or energy devices. The procedure restores a single, healthy cavity for future pregnancies.
Pre-IVF Cavity Assessment
A targeted hysteroscopy before an IVF cycle to confirm a normal, receptive uterine environment. Often performed alongside an endometrial scratch or biopsy when chronic endometritis is suspected.
Why Choose Dr. Rukkayal?
- MRCOG (UK) and FRM (Germany) trained — international expertise in fertility-focused uterine surgery.
- Diagnostic and operative hysteroscopy performed in the same sitting wherever clinically appropriate.
- Targeted, vision-guided tissue removal that protects healthy endometrium and future fertility.
- Direct integration with your IVF plan — uterine findings shape the next embryo transfer protocol.
- Same-day discharge with minimal pain and fast return to normal life.
- Honest, evidence-based counselling on when hysteroscopy will (and will not) improve your chances.
- Convenient Chennai locations — Egmore/Chetpet morning, Mylapore evening, Tambaram on select days.
Your Treatment Journey
Pre-Procedure Evaluation
Review of ultrasound, HSG, fertility history, and prior cycles. Pre-anaesthetic assessment and routine pre-operative blood tests are completed.
Procedure Day
Hysteroscopy is performed under short general anaesthesia or sedation in a fully equipped theatre. The procedure typically takes 15 to 45 minutes depending on whether operative work is needed.
Targeted Treatment
Polyps, fibroids, adhesions, or septae identified during the procedure are treated in the same sitting wherever safe to do so, avoiding the need for a second surgery.
Recovery & Discharge
Most patients are discharged the same day. Mild cramping and light spotting for 24 to 48 hours is normal. Detailed recovery instructions and a follow-up plan are provided before discharge.
Fertility Planning Follow-Up
A follow-up visit reviews intra-operative findings and histopathology (if tissue was sent), then outlines the next step — natural conception attempt, IUI, or IVF / embryo transfer.

Have Questions About Your Treatment?
Book a consultation with Dr. Rukkayal Fathima to understand your options and next steps.
Frequently Asked Questions
Hysteroscopy under general anaesthesia or sedation is painless during the procedure. Afterwards most women experience mild period-like cramping for a few hours and light spotting for a day or two — easily managed with simple oral pain medication.
No. Almost all hysteroscopies — both diagnostic and routine operative — are day-care procedures with same-day discharge, usually within a few hours of waking from anaesthesia.
If hysteroscopy identifies and corrects a polyp, submucosal fibroid, adhesion, or chronic endometritis, multiple studies suggest improved implantation and pregnancy rates in the next IVF cycle. If the cavity is normal, the procedure simply confirms that the uterus is not the limiting factor and you can transfer with confidence.
Most patients can try in the very next menstrual cycle after diagnostic hysteroscopy or simple polypectomy. After larger operative procedures (septum resection, adhesiolysis), Dr. Rukkayal usually recommends one to two cycles of healing before embryo transfer or natural attempt.
D&C (dilatation and curettage) is a blind procedure — tissue is scraped out without direct vision. Hysteroscopy is targeted — the surgeon sees exactly what is being removed. This precision protects healthy endometrium and is the modern standard for evaluating and treating intrauterine pathology.
Not every patient. Routine pre-IVF hysteroscopy is reserved for women with abnormal ultrasound findings, previous failed transfers, recurrent miscarriage, suspected adhesions, or a history of uterine surgery. Dr. Rukkayal will decide based on your individual scans and history.
Cost depends on whether the procedure is diagnostic or operative, the type of pathology being treated, anaesthesia type, and the hospital/clinic where it is performed. We share a clear, itemised estimate during the consultation so there are no surprises.
When performed by an experienced surgeon, hysteroscopy is one of the safest gynaecological procedures and does not harm ovarian reserve. The cervix is gently dilated and the cavity is examined and treated with care to preserve the endometrium for future pregnancy.
Yes. Subtle signs such as micropolyps, strawberry-pattern hyperaemia, and oedematous stroma can be seen during hysteroscopy and confirmed on biopsy. Treating chronic endometritis with targeted antibiotics has been shown to improve implantation in some women with recurrent IVF failure.
Sometimes. When both the uterine cavity and the pelvic anatomy need evaluation (for example, in unexplained infertility or suspected endometriosis with cavity findings), combined laparoscopy + hysteroscopy under a single anaesthesia is efficient and is offered when clinically appropriate.
Related Specialties
Endoscopy (Overview)
Hub page covering both laparoscopy and hysteroscopy options.
Laparoscopy Treatment
Minimally invasive abdominal procedures for endometriosis, fibroids, and tubal disease.
Recurrent Miscarriage
Evaluation and treatment for repeated pregnancy loss, often guided by hysteroscopy findings.
IVF Treatment
Pre-IVF cavity optimisation through hysteroscopy can improve implantation rates.
Related Articles
Laparoscopy vs Hysteroscopy: Key Differences
Laparoscopy vs Hysteroscopy explained by Chennai fertility specialist Dr. Rukkayal Fathima. Understand the differences & which is right for you.
10 min read
Fibroid Treatment Without Surgery
Explore non-surgical fibroid treatment options in Chennai, including medication, UAE, and lifestyle changes. Expert guide by Dr. Rukkayal Fathima.
8 min read
Endometrial Thickness for Pregnancy
Understand endometrial thickness for pregnancy and IVF success. Expert insights from Dr. Rukkayal, Chennai's leading fertility specialist.
8 min read
Hysteroscopy: What to Expect
Learn about hysteroscopy in Chennai: procedure, recovery, cost, and benefits. Expert guide by Dr. Rukkayal Fathima.
9 min read
Recurrent Miscarriage: Causes & Care
Understanding recurrent miscarriage in Chennai: causes, diagnosis, and treatment options with Dr. Rukkayal Fathima.
8 min read
Fibroids & Fertility: Impact & Treatment
Understanding uterine fibroids and fertility in Chennai. Learn about impact, diagnosis, and treatment options for pregnancy.
11 min read
Period After Hysteroscopy: What to Expect
Understand your menstrual cycle after hysteroscopy in Chennai. Learn about period delays, bleeding, and when to seek help.
7 min read
Ready to Get Started?
Book a consultation with Dr. Rukkayal Fathima about your treatment options
Book AppointmentBook Consultation
Consultation Booked!
Thank you for reaching out. Our team will contact you shortly to confirm your appointment.
Need urgent help? Call us