PGT Genetic Testing in Chennai
Preimplantation Genetic Testing (PGT-A, PGT-M, PGT-SR) integrated with IVF — Dr. Rukkayal’s direct embryology lab involvement supports precise, evidence-led embryo selection for couples at higher genetic or recurrent-loss risk.
Preimplantation Genetic Testing (PGT) is a laboratory technique applied during IVF in which a small number of cells are gently biopsied from a blastocyst-stage embryo and genetically analysed before transfer. PGT helps identify embryos that have the correct chromosome count (PGT-A), screens for a specific inherited single-gene disorder (PGT-M), or detects structural chromosomal rearrangements (PGT-SR). For carefully selected couples — those with recurrent IVF failure, recurrent miscarriage, advanced maternal age, or a known genetic condition — PGT can shorten the path to a healthy live birth and reduce the heartbreak of pregnancy loss.
PGT is not a routine add-on for every IVF patient. Used appropriately, however, it provides important clarity in situations where embryo quality cannot be judged on appearance alone. Dr. Rukkayal’s direct involvement in the embryology lab — a rare combination of clinician and lab-trained reproductive medicine specialist — means every PGT cycle is reviewed in detail: which embryos to biopsy, when to biopsy them, how to interpret mosaic results, and which embryo to transfer first. PGT samples are sent to internationally accredited genetics laboratories using next-generation sequencing (NGS), and results are explained to you in plain language alongside the clinical implications for transfer planning.
~60% per transfer
Euploid Transfer Pregnancy Rate
Significant
Reduced Miscarriage Risk
When PGT May Be Discussed
You should see a specialist if you experience:
- Two or more failed IVF cycles despite good-looking embryos
- Two or more first-trimester miscarriages
- Maternal age above 38 with multiple available embryos to test
- Either partner carries a genetic condition diagnosed via karyotype or carrier screening
- Prior pregnancy or child with a chromosomal disorder
- Strong family history of a known inherited disease
Understanding PGT-A, PGT-M, and PGT-SR
PGT-A (preimplantation genetic testing for aneuploidy) checks whether each embryo has the correct number of chromosomes — embryos with abnormal chromosome counts rarely implant and frequently miscarry. PGT-M (monogenic disorders) is used by couples who are known carriers of a specific inherited disease such as thalassemia, sickle cell disease, cystic fibrosis, or Huntington’s disease — embryos free of that specific condition are identified for transfer. PGT-SR (structural rearrangements) is for couples in which one partner carries a balanced translocation or inversion, situations associated with recurrent miscarriage. In all three, a few cells are biopsied from the trophectoderm (the outer cell layer that will form the placenta) of a day 5 or 6 blastocyst — never from the inner cell mass that becomes the baby — and embryos are vitrified while results are returned. The results then guide which embryo, if any, is suitable to transfer in a subsequent frozen embryo transfer cycle.
Who PGT Can Help

PGT Pathways We Offer
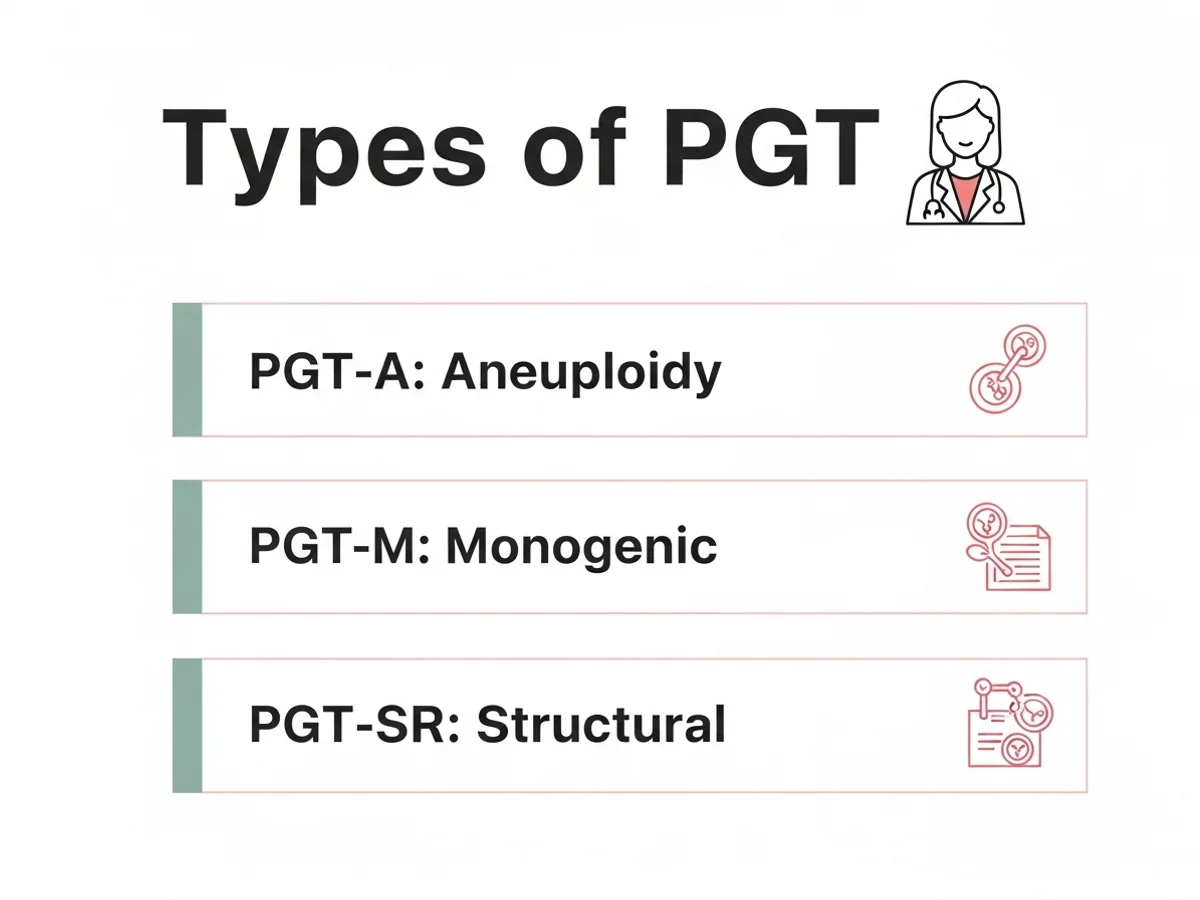
PGT-A (Aneuploidy Screening)
Next-generation-sequencing screen of all 23 chromosome pairs to identify chromosomally normal (euploid) embryos for transfer. Most relevant for women over 35, recurrent miscarriage, and recurrent IVF failure.
PGT-M (Single-Gene Disorders)
Targeted test for a specific inherited disease — for example, beta thalassemia, sickle cell disease, cystic fibrosis, or muscular dystrophy. Requires a pre-test workup to design a probe specific to the family.
PGT-SR (Structural Rearrangements)
Identifies embryos that have inherited a balanced or normal chromosomal pattern in couples where one partner carries a known translocation, inversion, or other structural variant.
Combined PGT-M + PGT-A
For couples needing both single-gene exclusion and chromosomal screening in the same cycle — for example, a thalassemia carrier couple over 35.
Sperm DNA Fragmentation Assessment
A complementary semen test that can inform whether PGT is likely to add value — high sperm DNA fragmentation is associated with higher aneuploidy rates and poorer embryo development.
Why Choose Dr. Rukkayal?
- Direct embryology-lab involvement — Dr. Rukkayal personally reviews embryo grading and PGT timing.
- Honest, evidence-based counselling on when PGT will help and when it will not.
- PGT samples processed at internationally accredited genetics laboratories using NGS.
- Clear, plain-language explanation of euploid, aneuploid, and mosaic results.
- Integrated frozen-embryo-transfer planning after PGT results are returned.
- FRM (Germany) and MRCOG (UK) trained — international reproductive medicine standards.
- Strict ICMR-compliant practice; no sex selection performed under any circumstances.
Your Treatment Journey
Genetic Counselling
A detailed consultation to confirm whether PGT is appropriate for your situation, what type of PGT applies, the expected information yield, the cost, and the limitations of the test.
IVF Cycle to Blastocyst
A standard or tailored IVF stimulation with the goal of producing multiple good-quality blastocysts on day 5 or 6, since PGT is only performed on blastocyst-stage embryos.
Biopsy & Vitrification
A few trophectoderm cells are biopsied from each suitable blastocyst by the embryologist and sent to the genetics lab. The embryos are vitrified (frozen) while results are awaited.
Results & Embryo Selection
Results are typically returned in 2–3 weeks. Dr. Rukkayal walks you through which embryos are euploid, mosaic, or aneuploid and recommends a transfer order based on your specific results.
Frozen Embryo Transfer
A planned, hormonally prepared frozen embryo transfer is scheduled in a subsequent cycle. Pregnancy and obstetric follow-up are coordinated thereafter.

Have Questions About Your Treatment?
Book a consultation with Dr. Rukkayal Fathima to understand your options and next steps.
Frequently Asked Questions
No. PGT in India is strictly regulated under the PC-PNDT Act. Sex selection is illegal and is not performed in our practice under any circumstances. PGT is used only for medical indications — chromosomal screening, single-gene disease, or structural rearrangements.
For carefully selected patients — older women, those with recurrent miscarriage, or those with recurrent IVF failure — PGT-A can reduce time-to-pregnancy and lower miscarriage rates by ensuring chromosomally normal embryos are transferred first. For younger women with normal egg quality, the benefit is smaller and the test is usually not recommended routinely.
When performed by an experienced embryologist on a true blastocyst-stage embryo, the trophectoderm biopsy is well-tolerated. The cells removed are from the outer layer that becomes the placenta, not from the inner cell mass that becomes the baby. Survival and implantation rates after biopsy are very close to those of unbiopsied embryos in good labs.
PGT cost is in addition to the IVF cycle cost and depends on the number of embryos tested and the type of PGT (A, M, SR, or combined). We share a clear itemised estimate covering the IVF cycle, the biopsy, the genetics-lab processing, and the subsequent frozen embryo transfer.
A mosaic embryo contains a mix of chromosomally normal and abnormal cells. Modern evidence shows that low-level mosaic embryos can sometimes implant and lead to healthy live births. The decision to transfer a mosaic embryo is made carefully with genetic counselling and informed consent.
Most laboratories return PGT-A results within 2–3 weeks. PGT-M is slower — the probe design step before the IVF cycle adds 6–12 weeks of preparation. We plan all of this into the timeline before starting your cycle.
Usually not. Most couples under 35 with no specific genetic or recurrent-loss history can proceed with standard IVF first. PGT is added when the medical indication justifies the additional cost and time.
No. PGT-A detects chromosome-count abnormalities. PGT-M detects only the specific disease for which the probe is designed. PGT cannot screen for every possible genetic condition, and a normal PGT result does not replace routine antenatal screening during pregnancy.
Related Specialties
IVF Treatment
Standard IVF cycle — the foundation on which PGT is added.
ICSI Treatment
ICSI is typically used for fertilisation when PGT is planned, to minimise contamination of the embryo sample.
Recurrent Miscarriage
PGT can reduce miscarriage rates in selected couples with recurrent loss.
Embryo Freezing & Vitrification
PGT-tested embryos are vitrified while results are awaited.
Related Articles
Age-Related Fertility Decline: Causes, Tests & Treatment Options
How age affects fertility in women and men. Dr. Rukkayal explains ovarian reserve, egg quality, AMH testing, and treatment options in Chennai.
11 min read
Chemical Pregnancy: Causes, Signs & Next Steps
What is a chemical pregnancy and why does it happen? Dr. Rukkayal explains causes, symptoms, recovery, and next steps for couples in Chennai.
10 min read
Donor Egg IVF: Is It Right For You?
Comprehensive guide to donor egg IVF in Chennai. Understand the process, success rates, and costs. Consult Dr. Rukkayal Fathima.
12 min read
Embryo Grading Explained
Understand embryo grading in IVF at Chennai clinics. Learn about the grading system and its impact on success.
10 min read
Fresh vs Frozen Embryo Transfer: Which Is Best?
Understand fresh vs frozen embryo transfer in Chennai. Learn about success rates, benefits, and which option is right for you.
10 min read
How Many IVF Cycles Are Needed?
Understand the average number of IVF cycles needed for success in Chennai. Dr. Rukkayal explains factors & success rates.
8 min read
IVF Failure: Common Reasons & Next Steps
Understand common IVF failure reasons in Chennai. Learn about causes, investigations, and next steps with Dr. Rukkayal Fathima.
8 min read
IVF Stimulation Protocol: What to Expect
Understanding the IVF stimulation protocol in Chennai: medications, process, and what to expect. Expert guidance from Dr. Rukkayal.
10 min read
Mini IVF vs Conventional IVF: Which Is Best?
Understand the key differences between Mini IVF and Conventional IVF in Chennai. Find out which option is right for you.
10 min read
Recurrent Miscarriage: Causes & Care
Understanding recurrent miscarriage in Chennai: causes, diagnosis, and treatment options with Dr. Rukkayal Fathima.
8 min read
Ready to Get Started?
Book a consultation with Dr. Rukkayal Fathima about your treatment options
Book AppointmentBook Consultation
Consultation Booked!
Thank you for reaching out. Our team will contact you shortly to confirm your appointment.
Need urgent help? Call us